Hip and Leg Pain Treatment
Chiropractic and rehabilitative care to reduce pain, improve alignment, and restore confident movement
Hip and Leg Pain Treatment
Chiropractic and rehabilitative care to reduce pain, improve alignment, and restore confident movement

Hip pain and leg pain often show up together because the hip, pelvis, and lower back control how force travels into the thigh, knee, and foot. When one area loses mobility or stability, the body compensates—then pain spreads. At Fairfax Station Chiropractic, we build a clear treatment plan that targets the real source (joint, disc, nerve, muscle, or movement pattern), not just the symptom location.
Hip pain and leg pain often show up together because the hip, pelvis, and lower back all work together when you stand, walk, bend, and move. When one area loses mobility or stability, the body starts to compensate, and pain can spread. Dr. Christopher Virusky creates treatment plans that focus on the real source of the problem, not just where the pain shows up.
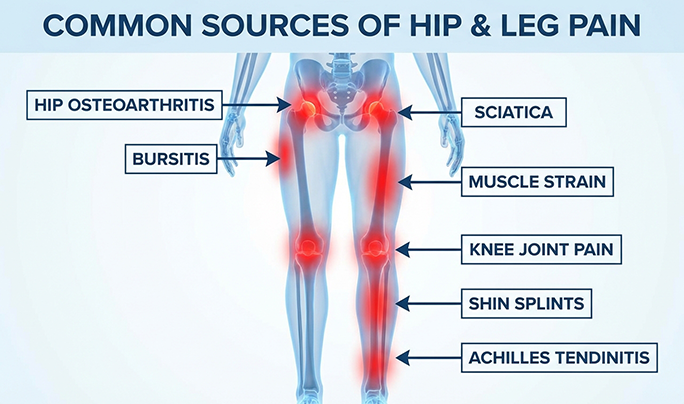
Common Sources of Hip and Leg Pain
Hip-related drivers we commonly evaluate:
- Hip osteoarthritis causing stiffness, grinding, and reduced range of motion
- Trochanteric bursitis producing outer-hip pain and tenderness
- Labral irritation or soft tissue strain causing catching or instability
- Muscle guarding and trigger points in glutes, hip flexors, and IT band
Referred or radiating sources that mimic hip pain:
- Sacroiliac and pelvic alignment issues altering load distribution
- Lumbar disc irritation or nerve compression producing thigh/calf symptoms
- Movement compensation from weak glutes/core or restricted ankle mobility
Leg pain drivers we commonly evaluate:
- Nerve irritation (sciatic-type patterns: sharp, electric, burning)
- Overuse and strain (standing jobs, sudden mileage increases, repetitive work)
- Muscle imbalance and core fatigue affecting gait stability
- Degenerative changes (disc thinning, arthritis, facet irritation)
- Circulatory/metabolic contributors that slow healing or cause swelling
If symptoms include visible swelling, warmth, color changes, or sudden severe calf pain, evaluation is important to rule out vascular concerns.
Symptoms We Pay Close Attention To
- Groin, buttock, or outer-hip aching that worsens after standing or walking
- Sharp pain with stairs, standing from a chair, or getting out of a car
- Clicking, popping, catching, or locking sensations in the hip
- Numbness, tingling, burning, or weakness traveling down the thigh/leg
- Morning stiffness or tightness after sitting or driving
- Limping, balance changes, or difficulty with single-leg tasks (shoes, step )
- Night cramps, restless-leg sensations, or throbbing that disrupts sleep
Tracking what triggers symptoms (sitting, driving, walking hills, workouts) helps us fine-tune the plan faster.
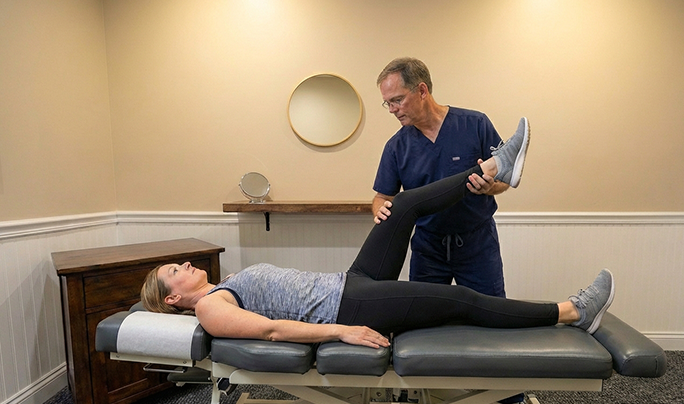
Our Collaborative Evaluation
We start with a full-body approach because hip and leg pain are rarely isolated.
- Health history review (injury, work demands, sleep habits, footwear, training)
- Functional testing (gait, balance, strength, mobility, orthopedic screens)
- Neurological testing when radiating pain or weakness is present
- Imaging coordination (X-ray/MRI/ultrasound) when clinically indicated
- Goal-based planning with progress checks (ROM, strength, functional markers)

Treatment Options We Use
Chiropractic Adjustments
Gentle corrections for the lumbar spine, SI joint, pelvis, and hip mechanics to improve alignment, reduce joint stress, and calm nerve irritation.
Corrective Exercise and Therapy
Progressive stability and mobility work focused on glute activation, core strength, hip control, and movement retraining.
Soft Tissue Release and Massage Therapy
Myofascial release, trigger point work, and instrument-assisted techniques to reduce adhesions, improve circulation, and decrease chronic guarding.
Electrotherapy and Ultrasound
Supportive modalities to reduce irritation and help tissue recovery during flare-ups.
Lifestyle and Ergonomic Coaching
Practical changes for desk setup, driving posture, sleep positioning, footwear, and activity modification to reduce reinjury risk.
A Simple Recovery Roadmap
Relief Phase
Reduce pain, calm inflammation, and restore baseline mobility.
Correction Phase
Fix movement faults, rebuild strength, and improve load distribution.
Prevention Phase
Maintain alignment, reinforce mobility habits, and reduce flare-ups long-term.
- More info
Acupuncture & Dry Needling: Needle-based techniques calm inflammation, modulate pain signals, and encourage healing.
Electrotherapy: Electrical stimulation decreases swelling, improves muscle activation, and promotes tissue repair.
Spinal Decompression: Non-surgical traction relieves pressure on discs and facet joints, especially helpful for spinal arthritis.
Trigger Point Injections: In collaboration with licensed providers, injections release stubborn muscle knots associated with arthritic pain.
Vibration & Balance Therapy: Whole-body vibration improves circulation, proprioception, and mobility—excellent for stiffness and fall prevention.
Regenerative Treatments (via referral): Advanced options such as platelet-rich plasma (PRP) or A2M therapy may protect cartilage and support repair when conservative care alone isn’t enough.
Each plan is unique. We combine therapies in the sequence and frequency that best fit your body, schedule, and goals.

Frequently Asked Questions
- Q: How soon will I feel better?
A: Many patients notice changes early, but timelines depend on severity, duration, and how much daily stress is hitting the hip/leg.
- Q: Can I stay active during treatment?
A: Often yes. We usually modify activity instead of stopping it completely, based on your exam.
- Q: Do you accept insurance?
A: If you don’t see your provider listed, call and we can verify benefits.
- Q: Am I a candidate?
A: Most patients with mechanical hip pain, gait-related leg pain, or nerve irritation patterns benefit from conservative care—especially when addressed early.
