Joint Pain and Arthritis Treatment
Non-surgical care focused on reducing inflammation, restoring mobility, and protecting long-term joint function.
Joint Pain and Arthritis Treatment
Non-surgical care focused on reducing inflammation, restoring mobility, and protecting long-term joint function.

Joint pain and arthritis often overlap, but they are not the same thing. Many people deal with stiffness, aching, or instability long before they are officially told they have arthritis. Dr. Christopher Virusky focuses on finding the movement, joint, and inflammation-related factors behind the discomfort, then creating a care plan that helps improve function and make daily life easier.
Understanding Joint Pain and Arthritis
Joints allow movement, absorb stress, and stabilize the body. Pain typically emerges when cartilage wears down, tissues become inflamed, or muscular support weakens.
Joint irritation may be linked to:
- Degenerative joint changes
- Inflammatory processes
- Repetitive mechanical stress
- Prior injuries or surgeries
- Postural and movement habits
- Autoimmune conditions
- Sedentary lifestyle patterns
Arthritis, by contrast, refers to a group of conditions involving joint inflammation and progressive tissue changes. While there is no single cure for every form of arthritis, symptoms and day-to-day function can often be managed with conservative care.


Common Symptoms Patients Report
- Persistent aching or stiffness
- Morning tightness or startup pain
- Swelling or joint sensitivity
- Sharp pain with movement or loading
- Clicking, popping, or grinding sensations
- Instability or weakness near the joint
- Reduced range of motion
These patterns frequently affect knees, hips, shoulders, wrists, ankles, and the spine.
Arthritis Conditions We Commonly Manage
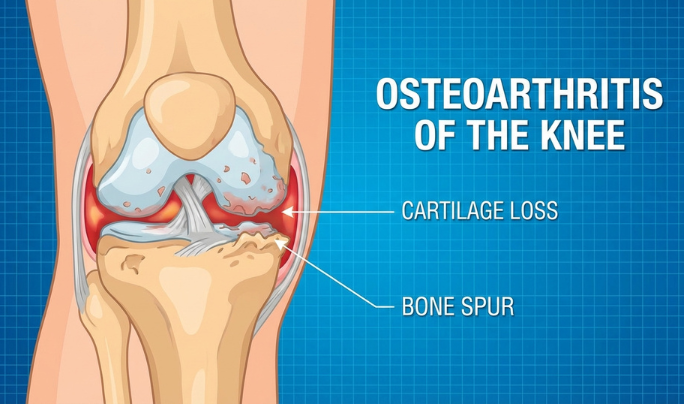
Osteoarthritis (OA)
Age-related cartilage wear leading to stiffness and mechanical pain commonly affects knees, hips, hands, and the spine.
Rheumatoid Arthritis (RA)
Autoimmune-driven joint inflammation that may involve multiple joints and fluctuating symptom intensity.
Inflammatory Arthropathies
Conditions such as gout or psoriatic arthritis produce episodic swelling and pain.
Post-Traumatic Arthritis
Degenerative changes following injury or repetitive joint stress.
Each presentation differs, which is why individualized assessment is essential.
Our Treatment Philosophy
Care focuses on improving joint mechanics, reducing inflammatory stress, and reinforcing movement stability.
Chiropractic Adjustments
Targeted joint and spinal corrections help improve alignment, motion, and load distribution.
Soft Tissue Therapies
Myofascial release and manual techniques reduce muscular tension contributing to joint compression.
Corrective Exercise and Rehabilitation
Strength and mobility programs enhance joint stability and resilience.
Joint Mobilization Techniques
Controlled movement strategies help restore flexibility in restricted joints.
Therapeutic Modalities
Electrotherapy and related approaches may be used to calm irritation and support tissue recovery.
Lifestyle and Ergonomic Guidance
Movement habits, workstation setup, sleep positioning, and activity modification are addressed to reduce recurring strain.
For complex cases, care may be coordinated alongside other medical providers when appropriate.
Why Early Care Matters
Joint dysfunction tends to progress when movement patterns remain unchanged. Early conservative care may help:
- Reduce chronic inflammation cycles
- Preserve joint mobility
- Improve weight-bearing mechanics
- Decrease compensation injuries
- Support long-term activity tolerance
- More info
Acupuncture & Dry Needling: Needle-based techniques calm inflammation, modulate pain signals, and encourage healing.
Electrotherapy: Electrical stimulation decreases swelling, improves muscle activation, and promotes tissue repair.
Spinal Decompression: Non-surgical traction relieves pressure on discs and facet joints, especially helpful for spinal arthritis.
Trigger Point Injections: In collaboration with licensed providers, injections release stubborn muscle knots associated with arthritic pain.
Vibration & Balance Therapy: Whole-body vibration improves circulation, proprioception, and mobility—excellent for stiffness and fall prevention.
Regenerative Treatments (via referral): Advanced options such as platelet-rich plasma (PRP) or A2M therapy may protect cartilage and support repair when conservative care alone isn’t enough.
Each plan is unique. We combine therapies in the sequence and frequency that best fit your body, schedule, and goals.

Frequently Asked Questions
- Q: How quickly will I notice improvement?
A: Response times vary depending on severity, tissue health, and daily stressors affecting the joint.
- Q: Are treatments non-surgical?
A: Yes. Care emphasizes conservative, movement-based strategies.
- Q: Can this help if I already have arthritis?
A: Many patients with arthritis benefit from mobility, strength, and inflammation-focused management.
- Q: Is care customized?
A: Always. Plans reflect examination findings, tolerance levels, and functional goals.
